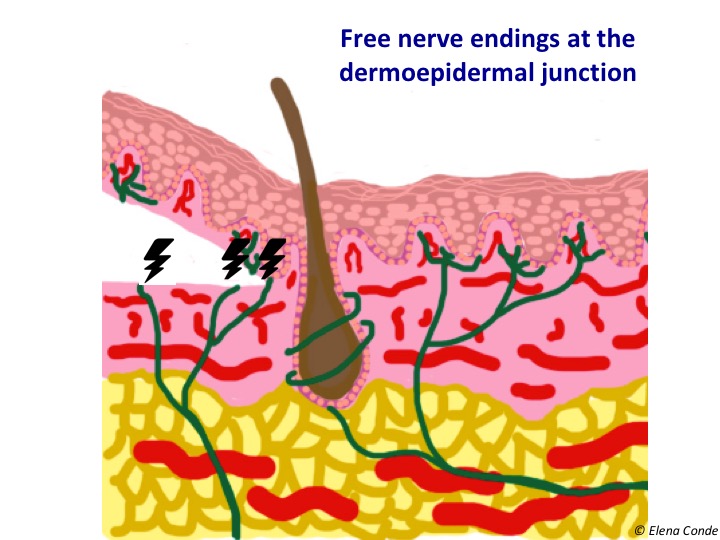
Given the varying etiologies and incompletely identified molecular mechanisms resulting in neuropathic pain, investigation into immune system involvement has received much attention ( 9, 10). 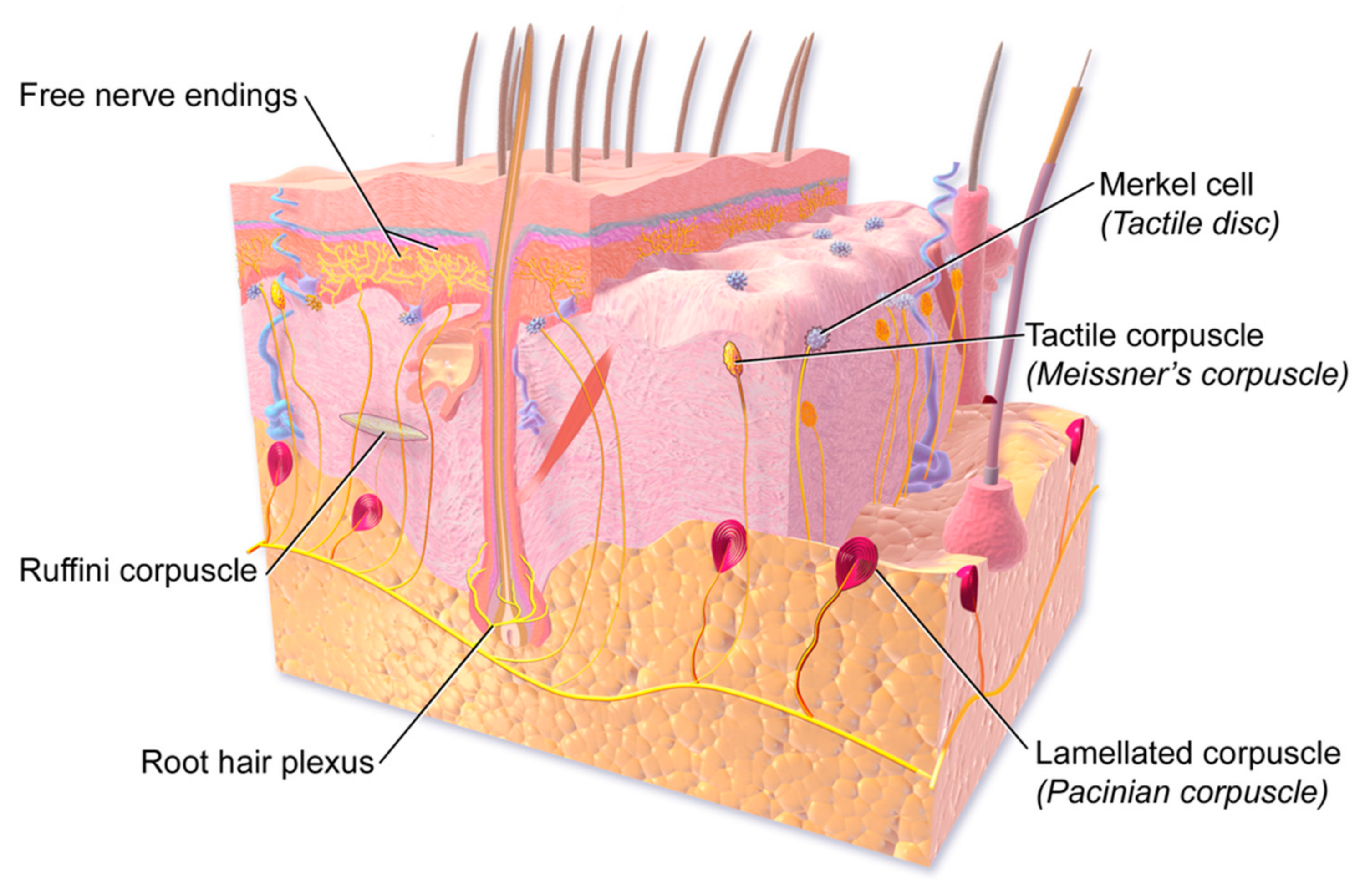
Neuropathic pain refers to pathological pain generated in response to lesion or disease of the somatosensory system ( 8). It has increasingly become clear that a significant neuroimmune component also contributes to the pathogenesis of neuropathic pain ( 7). While cutaneous neuroimmune interactions are critical in healthy host physiology, their dysregulation is implicated in many disease states, notably psoriasis ( 3), atopic dermatitis (AD) ( 4) and allergic contact dermatitis (ACD) ( 5, 6). Analogously, nerve terminals can release a cocktail of neuropeptides which modulate immune cell function ( 2). Upon activation, immune cells release a myriad of inflammatory mediators and intercellular messenger chemicals, which can stimulate sensory nerve terminals in the skin. Concurrently, cutaneous sensory neurons detect tissue damage and other external stimuli, relaying this information to the central nervous system (CNS).įar from operating in isolation, tremendous crosstalk occurs between the peripheral sensory nervous system and the immune system. Physical structure, antimicrobial biomolecules and immune cell function are among the defensive modalities employed by the skin to protect the host from invasion. An intricate network of immune and non-immune cells is responsible for maintaining tissue homeostasis, responding to harmful challenges and promoting tissue repair. 
Modern understanding acknowledges the skin as a highly complex protective network against external physical, chemical, and microbiological insult. No longer is the skin regarded a purely physical barrier separating an organism from its environment ( 1). 
Finally, we highlight the future promise of emerging therapies associated with skin neuroimmune crosstalk in neuropathic pain. We then summarize evidence of neuroimmune mechanisms in the skin in the context of peripheral neuropathic pain states, including chemotherapy-induced peripheral neuropathy, diabetic polyneuropathy, post-herpetic neuralgia, HIV-induced neuropathy, as well as entrapment and traumatic neuropathies. In particular, we discuss recent findings concerning neuroimmune communication in skin infections, psoriasis, allergic contact dermatitis and atopic dermatitis. We discuss modulation of cutaneous immune response by sensory neurons and their mediators (e.g., nociceptor-derived neuropeptides), and sensory neuron regulation by cutaneous immune cells (e.g., nociceptor sensitization by immune-derived mediators). Herein, we provide an overview of the sensory innervation of the skin and immune cells resident to the skin. The skin is a highly complex biological structure within which peripheral sensory nerve terminals and immune cells colocalise. Dysregulation of this delicate physiological balance is implicated in the pathological mechanisms of various skin disorders and peripheral neuropathies. This crosstalk is facilitated by a variety of cytokines, inflammatory mediators and neuropeptides. School of Medical Sciences, The University of New South Wales, UNSW Sydney, Sydney, NSW, Australiaīidirectional interplay between the peripheral immune and nervous systems plays a crucial role in maintaining homeostasis and responding to noxious stimuli.
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
